Cellular signaling drives stem cells to form bone
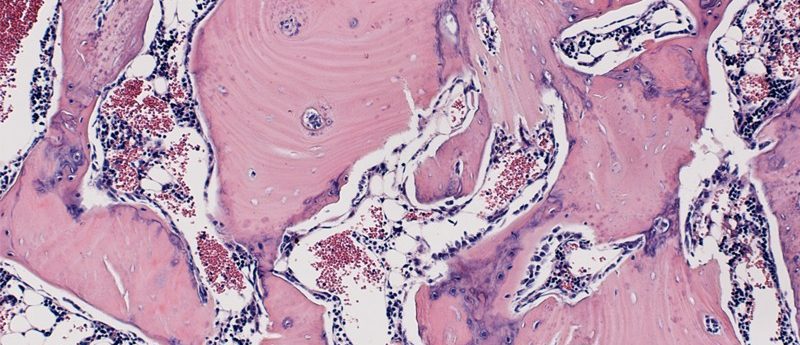
Fat and bone stem cells have been found to preferentially favor bone repair when signaling from a key cellular protein, WISP-1, is manipulated.
Bone formation in the rat spine. Credit: Aaron James, Johns Hopkins Medicine
Researchers from Johns Hopkins University School of Medicine have found evidence that signaling from a particular protein — WISP-1 — can manipulated to drive perivascular stem cells that would normally form both fat and bone to favor building bone tissue. This could be harnessed to prevent bone loss due to aging and speed recovery after surgery or fracture.
“Our bones have a limited pool of stem cells to draw from to create new bone,” commented Aaron James, associate professor of pathology at the Johns Hopkins University School of Medicine (MD, USA), and the study’s senior author. “If we could coax these cells toward a bone cell fate and away from fat, it would be a great advancement in our ability to promote bone health and healing.”
Approximately 1.5 million Americans suffer fractures as a result of bone disease each year and around 391,000 Americans receive spinal fusions, a process whereby vertebrae are fused to relieve pain or restore mobility, which requires huge amounts of new bone cells.
In the study, James and his team engineered human fat cells to over-express WISP-1 and found that “bone-driving” gene became twice as active, whilst the activity of “fat-driving” genes such as peroxisome proliferator-activated receptor gamma (PPARγ) decreased by 42%. In a rodent model of spinal fusion, rats treating with these cells experienced new bone forming, whereas control rats did not experience bone fusion in the time they were observed.
“We hope our findings will advance the development of cellular therapies to promote bone formation after surgeries like this one and for other skeletal injuries and diseases, such as broken bones and osteoporosis,” said James.